| ||||
What Are Bacterial Fimbriae?
Structure, Function & Relationship to Bacterial Virulence
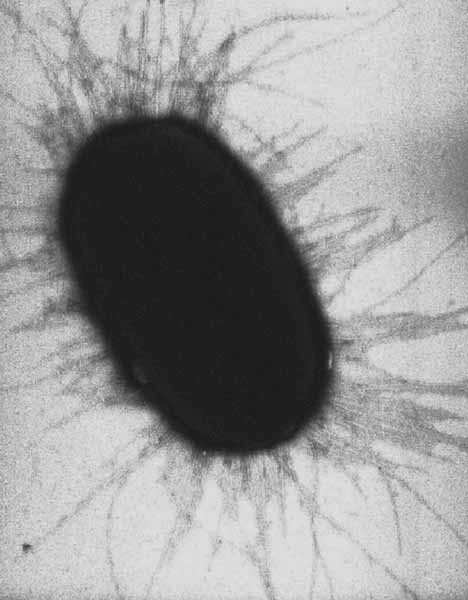
Many bacteria, particularly those with Gram-negative cell wall structure, have external appendages; delicate strands of protein that extend beyond the surface of the cell. These external structures of bacteria can come in many forms.
Article Summary: Most Gram-negative bacteria have fimbriae; hair-like projections, external to the cell wall, that allow bacteria to stick to the cells they infect.
What Are Bacterial Fimbriae?
You have free access to a large collection of materials used in a college-level introductory microbiology course. The Virtual Microbiology Classroom provides a wide range of free educational resources including PowerPoint Lectures, Study Guides, Review Questions and Practice Test Questions.
SPO VIRTUAL CLASSROOMS
 | ||||||
How Fimbriae Help Bacteria Cause Disease
Fimbriae are a major factor in bacterial virulence (the ability of a bacterium to cause disease), since these structures enable some bacteria to colonize human epithelial cells (cells of mucous membranes).
At the end of each fimbria are special proteins called adhesins. The specific type of adhesin varies by type of bacteria, but regardless of the type, adhesin molecules allow bacteria with fimbriae to adhere to host cells by docking, like a lock and key, with receptor proteins on the surface of host epithelial cells.
This ability of fimbriae to stick to epithilial cells leads to many diseases transmitted via mucous membranes, including gonorrhoeae, bacterial meningitis and infections of internal medical devices and indwelling catheters. The following are descriptions of three species of pathogenic bacteria that rely on their fimbriae to cause disease.
Page last updated:
9/2015
The SPO website is best viewed in Google Chrome,
Microsoft Explorer or Apple Safari.
Long, thin flagella are used by some bacteria to move about. Sex pili allow bacteria to share genes. Shorter extensions, called fimbriae (singular fimbria), enable bacteria to adhere to surfaces and potentially infect the cells of their host.
Gram-negative Bacterial Fimbriae
Most Gram-negative bacteria have these short, fine appendages surrounding the cell. In contrast, Gram-positive bacteria never have fimbriae.
These protein projections are not used to help the cell move about, but instead make it possible for bacteria adhere to each other, surfaces and to host cells. Basically fimbriae help bacteria stick to things.
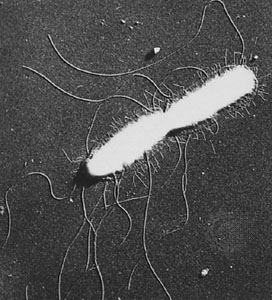
Electron micrograph of Salmonella bacteria showing both flagella (long extensions) and fimbriae (short extensions).
 | ||||||
SPO is a FREE science education website. Donations are key in helping us provide this resource with fewer ads.
Please help!
(This donation link uses PayPal on a secure connection.)